THE DALLES — Wasco County wants to change the way it contracts for ambulance service providers. But current providers don’t like the draft plan, describing it as concerning, a disaster, and flat out unacceptable. They also say it was developed without their input and away from public view.
County Administrator Tyler Stone says the current system has holes that must be fixed, such as areas that can’t provide their own ambulance service and repeated struggles to provide reliable service taking non-emergency patients from The Dalles’ hospital to other facilities, including in Portland.
It’s a heated and long-running dispute, and one resolution could see a private company from outside the region, such as Metro West, overseeing local ambulance services — a potentially significant change.
How ambulance service works now
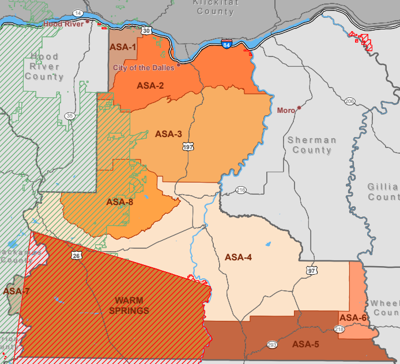
In Oregon, counties must make sure ambulance services are available everywhere. Currently, Wasco’s ambulance plan divides the county into eight service areas, and the county signs contracts with different local providers for each.
For example, Mid-Columbia Fire & Rescue, which employs only professional staff, does ambulance coverage in the county’s most populous area, including The Dalles, while the all-volunteer Wamic Rural Fire Protection District provides ambulance service for about 650 permanent residents — a population that can swell to much larger on weekends.
Mosier gets ambulance coverage from Hood River Fire & EMS, part of southern Wasco County is served by first responders from Jefferson County, and Dufur has sought waivers to staffing and certification requirements for its volunteer ambulance service.
Wasco County Emergency Manager Sheridan McClellan noted the variety of Ambulance Service Areas (ASAs) in a July 16 email to providers explaining the new plan. “Some are healthy and doing great,” McClellan wrote, “and one is currently not functioning, with the remainder somewhere in between.”
All ambulance agencies in the county have mutual aid agreements with each other to give extra help when needed. The county board of commissioners is ultimately responsible for ensuring ambulances are available when residents need them, and setting required response times and minimum equipment and staffing standards.
What the county plan would change
Wasco County’s proposed plan would offer just one county-wide contract instead of separate contracts per service area, and have the winning bidder seek subcontracts with existing providers for local services.
“The purpose of this structure is to preserve existing rural providers, preserve their revenue sources, build depth in the system, and take advantage of economies of scale,” the new county plan says, citing examples of efficiencies such as rural areas co-staffing calls, sharing the cost of a required medical director, loaning out ambulances and buying supplies in bulk.
In June, the Oregon Health Authority (OHA) approved the plan as meeting legal requirements. But Stone calls it a draft that has to be put out to bid and responses evaluated. “I think we have a problem if we’re unwilling to look at all the possible alternatives that could make this a better program,” he said. “It could be this is a terrible approach or it could be that this is a phenomenal approach that could be adopted statewide. But we don’t know until we ask the question.”
Stone says the two big challenges with ambulance service the county has had over the last several years are “non-emergency” ambulance transportation, and the struggle in some small communities to recruit and keep enough volunteers.
What’s at stake
But ambulance service providers in Wasco County are skeptical of big savings with a single contractor, and say volunteers go through a natural ebb-and-flow cycle.
Mid-Columbia Fire & Rescue Chief David Jensen says his main concern is that if a private contractor won the contract, it would need to make a profit, and if it could not, it would leave, potentially after current local providers had shut down and dismantled. “Our whole county would be left in the lurch,” Jensen told Uplift Local.
Ambulance services are funded by health care dollars; providers bill insurance companies. But fire services are paid for by local taxpayers. Jensen says that only by combining both sources of revenue can Mid-Columbia Fire & Rescue provide its current levels of services. He also worries that local ambulance dollars might wind up subsidizing other parts of the county, if one provider managed the whole county.
“Rural providers may, in effect, share the revenue from [The Dalles area], and will add to the depth and quality of ambulance services throughout the county,” the new plan says.
Stone shares Jensen’s concern that an outside provider could potentially lead to the dismantling of local infrastructure. But he says that risk is higher under the current system, where providers can bid on just one service area, instead of tying the fortunes of those that are struggling to the high-performers by creating one ambulance district to manage the entire county. And he says if outside companies bid under either approach, state law says the county can’t legally favor a current provider — applicants have to be evaluated on their ability to do the required jobs.
Stone suggests a potential example of how single-agency management might distribute resources effectively: offering stipends to volunteers in small districts when they drive a patient from The Dalles to Portland. He says rural providers can spell out their needs when they subcontract.
But in tiny Wamic, in south Wasco County, Fire Chief Larry Magill called one county-wide contract a “nonstarter” that would hurt his community. “I would have no control,” he said, painting a scenario in which the primary contractor might require his volunteers to backfill in other places, not due to an emergency, but simply if staffing ran short.
“The small-community mentality of helping your neighbor would go away,” Magill said.
Problems with process
Chief Jensen informed his district’s board about the county’s new plan at its July 21 meeting. He said had first seen the new plan just days earlier, on July 16, the same day OHA approved it and Wasco County’s emergency manager shared it with ambulance service providers.
Jensen described what he saw as “nowhere near the same plan” that service providers had agreed on with the county emergency services department and had been submitted for OHA approval in late 2024.
But that plan “was returned for further development,” McClellan explained to service providers in a July 22 email. “It did not provide solutions for ensuring coverage.”
County Administrator Stone acknowledged that the plan came back “different” after the state review compared to what had been discussed with providers. But he said the challenges were known, and the changes shouldn’t have been a surprise. “We’ve been looking at a single provider approach for sometime now,” he told Uplift Local.
Providers fired back in emails to McClellan after he shared the revised plan with them.
“It seems the county is completely disregarding the work we put in last year,” Jensen wrote to McClellan on July 23. “Most concerning is that the county did so secretly, without any consultation with the ASA committee and without receiving any input from impacted agencies.”
“I feel the county administration has overstepped and went around the county providers,” Wamic’s Chief Magill wrote. “My recommendation is that this process needs to stop immediately and have a meeting with the ASA committee to get the plan back onto track that was agreed upon last year.”
“I am becoming a bit annoyed with these slight tactics to attempt to lure the committee from what we agreed on,” Michael Lepin, deputy chief of emergency management services in Jefferson County, wrote.
“Evidently we are not getting the point to or across to whoever is directing you and you are not listening,” Juniper Flat Rural Fire Protection District Chief Eugene Walters wrote. “Getting the approval from OHA, all done without the ASA committee discussions is on the edge of being corrupt or at least not done in order of professional procedures on behalf of the citizens of Wasco Co.”
“This should be a public process,” Hood River Fire Chief Leonard Damian wrote.
Stone says the process is public, and not over. “We ran it through OHA to see if it was an acceptable approach, and we brought it back to providers,” he said, referring to a July 22 meeting in Maupin with service providers, noting that there are “several more steps” before the plan could be approved.
The non-emergency transfers thorn
The draft plan also singles out The Dalles area, now served by Mid-Columbia Fire & Rescue. It says that the county-wide provider’s responsibilities would include ensuring transport of patients from Adventist Health Columbia Gorge (formerly Mid-Columbia Medical Center) to other facilities and overseeing county employee EMS training.
The ambulance service known as “non-emergency transfers” is a critical issue in this dispute. In addition to emergency services, ambulances drive people from hospitals back home, to rehab facilities, or to other hospitals. The term includes sometimes urgent, but not critical care.
In Wasco County, most of this non-emergency work falls to Mid-Columbia Fire & Rescue because it serves The Dalles, home to the county’s only hospital. The dispute centers around taking patients from Adventist Health Columbia Gorge to facilities in Portland or other towns.
Under current rules, the hospital must first offer non-emergency jobs to the local ambulance provider, but is ultimately responsible for finding that transport itself. But in 2021, then Mid-Columbia Medical Center raised concerns over that language, which was relatively new, citing several situations when Mid-Columbia Fire & Rescue declined transfers, including during red-flag fire warnings, inclement weather, and a request to take a patient to Bend.
The hospital suggested that the agency add staff or activate mutual aid agreements with other providers so local ambulance crews could take patients to out-of-town facilities. Then last year, Mid-Columbia Fire & Rescue wrote a letter to the medical center saying it would stop doing non-emergency out-of-town transfers because they were an “ongoing challenge” due to changes in medical services locally, including lower hospital staffing.
The new draft county plan aims to plug that transport hole, requiring ambulance services be provided to The Dalles’ hospital, including non-emergency and inter-facility transfers.
“We need the transfer services to happen,” Stone told Uplift Local. “I’m having a hard time understanding why they’re having trouble doing it now when literally they’ve done it for decades.”
He says more expensive helicopter flights aren’t the best answer.
But Jensen told Uplift Local the only issue for his agency is sending ambulance crews to Portland, which puts his staff “out of commission” and unavailable for local emergencies for hours, he said. He also said Mid-Columbia Fire & Rescue is in conversation with the hospital about possible alternatives, including contracting directly with a different ambulance provider, getting its own ambulance, co-staffing some transports with MCFR, or changing the times when “non-emergency” trips are scheduled.
Jensen says the county’s proposed plan would take his negotiating leverage away.
A confusing committee
In their criticism of the process, several ambulance service providers said the county went around the “ASA committee.” According to Wasco County’s current ambulance service plan, a public Ambulance Service Area Review Committee oversees updates to ambulance services. The committee is sprawling, listing as members an unspecified number of emergency room doctors and nurses, members of the public from each of the eight ambulance service areas, and all ambulance service providers.
But unlike elsewhere in Oregon, where ambulance review committees meet regularly and publish agendas and minutes, Wasco County’s ambulance review committee has operated on a more ad hoc basis, meeting as the emergency service manager saw fit, and sometimes conversing over email.
The county’s new plan proposes shrinking the committee, in part by allotting just two provider seats at the table instead of a representative of each.
What comes next
Although OHA has approved the county’s draft plan, the Wasco County Board of Commissioners has not, and that must happen before any contracts can be put out to bid.
The next step is working through the draft proposal with providers, who say they are unified against a subcontracting system. County Emergency Manager McClellan told Uplift Local that an ambulance review committee meeting scheduled for Sept. 17 was postponed “due to a lack of availability from providers and members.” A meeting is expected to happen later this fall; the conversation may influence recommendations to county commissioners.
•••
Find more Uplift Local stories at upliftlocal.news/columbia-gorge. See Documenter Swen Carlson’s full notes at columbia-gorge.documenters.org.





















Commented